Don’t let fear delay vital emergency care
“We’ve gone above and beyond to keep the ER sterile,” says Dr. Chris Fox, chair of the Department of Emergency Medicine at the UCI School of Medicine.
Photo by Carlos Puma
Dr. Chris Fox wasn’t worried that his wife would be exposed to the virus that causes COVID-19 when he brought her to UCI Medical Center’s emergency room for X-rays after a recent cycling accident.
Fox, chair of the UCI School of Medicine’s Department of Emergency Medicine, feels safer in the emergency room (ER) he directs than he does walking through any local store. But he knows others may be fearful.
“We’ve gone above and beyond to keep the ER sterile,” Fox says. “But after COVID-19 started to ramp up, patients became afraid to see their primary care providers or come to the hospital.”
ER visits dropped by one-third
Almost overnight, visits to the UCI Medical Center ER dropped by a third when the COVID-19 crisis hit in March. Those who did come were much sicker and in more desperate condition because they had delayed seeking care.
People with diabetes who shied away from seeing their primary doctors were ending up in the ER with life-threatening ketoacidosis. Others who delayed seeking care for chest pain or stroke symptoms were left with fewer treatment options, Fox says.
One person had an inflamed appendix that ruptured. Another patient’s skin infection threatened to spread to the blood stream, which could lead to a potentially life-threatening condition called sepsis or even a bone marrow infection that could require amputation.
“In the ER, we went from seeing 150 patients per day to 100,” Fox says. “Now we’re seeing about 125 a day, but we’re admitting many more of them directly to the hospital because of the severity of their condition.”
Is it an emergency?
It’s difficult for people to know when to seek emergency care, but Fox says it’s better to come in than not.
Go to the ER if your symptoms include:
- Sudden weakness
- Blurred or sudden loss of vision
- Chest pain
- Shortness of breath
- Abdominal pain
- Fever, especially with back, chest or abdominal pain
- Broken bone
- Painful red rash
Preventing COVID-19
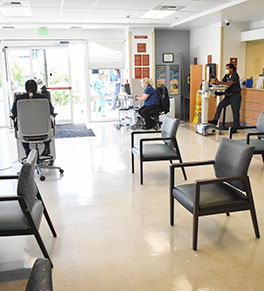
The medical center’s ER looks different today since operations were restructured to prevent the spread of COVID-19.
Key changes include:
- Screening all patients for fever and other symptoms of COVID-19. People who have symptoms or may have been exposed to the virus are isolated in individual rooms for testing. Results are ready within two hours.
- All ER staff — which at any one time includes six doctors, two nurse practitioners, 25 registered nurses and dozens of support staff — are screened daily for COVID-19.
- All staff wear masks and other protective clothing.
- All patients are given masks if they don’t already have them.
- The entire ER and the waiting room are cleaned thoroughly every hour.
- The waiting room is configured to keep people at least six feet apart, limiting capacity to 14. Backup plans are in place to accommodate more when needed.
Learn more about UCI Health COVID-19 safety practices ›
Patients feel safer
These very visible changes have allayed many patients’ fears, according to Fox.
“Because we have streamlined the process of assessing patients and splitting people who are suspected of having COVID-19 from those who are not, our patients feel safer,” he says. “This also has resulted in a big uptick in patient satisfaction scores.”
Given all the precautions, Fox was confident that it was safe to bring his wife to the medical center’s ER to learn whether she had been seriously injured in the cycling accident. Once he read her X-rays, both were relieved when they turned out to be normal.
“I had zero concerns about bringing my wife into the ER,” he says. “I practice what I preach.”




