Delaying stroke care can be deadly
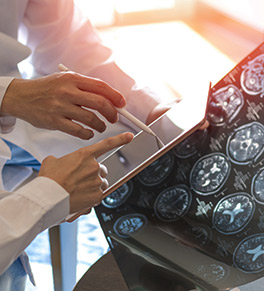
Stroke experts have a saying: “Time is brain.”
It means that delays in getting care when experiencing stroke symptoms reduces a patient’s treatment options and increases the risk of lasting disability or death, says vascular neurologist Mohammad Shafie, MD, PhD, associate director of the UCI Health Comprehensive Stroke and Cerebrovascular Center.
A recent study found that early in the COVID-19 pandemic, not as many people sought care when experiencing signs and symptoms of stroke than during the same period a year earlier. And those who did seek treatment arrived at hospitals 160 minutes later when compared to the same period in 2019. This delay is significant because the optimal time for giving clot-busting medications is under four hours.
UCI Medical Center saw a similar drop in patients seeking care as the pandemic started last spring, says Shafie, who is also an assistant professor of neurology at the UCI School of Medicine. “After the first three months or so, things began to normalize and people began to come in as usual.”
'Time is brain’
When a clot cuts off life-giving oxygen in blood flow to the brain as happens with an ischemic stroke — by far the most common type — up to two million brain cells per minute can be destroyed. The result may be neurological, cognitive and physical disability or death.
The longer the blockage, the greater the damage. That's why it's critical to get medical help as quickly as possible when signs and symptoms appear, Shafie says.
Any sudden onset of the following, alone or in combination, could indicate an imminent stroke:
- Facial drooping on one side
- Weakness in arm, leg or both on one side
- Numbness in arm, leg or both on one side
- Speech difficulties, including slurring words, trouble finding words or understanding others
- Severe headache (i.e., “worst headache of my life”) without any history or cause
- Dizziness or balance problems
- Vision difficulty, including double or blurred vision, transient loss of vision or trouble with peripheral vision in one eye
If you experience any of these symptoms or are with someone who is displaying them, call 9-1-1. "Even if you’re not one-hundred percent sure, call 9-1-1," Shafie says.
“Paramedics will assess the situation and transport the patient to the most appropriate care facility, such as the comprehensive stroke care center at UCI Medical Center, where our trained stroke specialists can help immediately.”
Early treatment is key
If a clot is the cause of your stroke, doctors can determine if you would benefit from a clot-busting drug called tissue plasminogen activator (tPA).
This medication can help reopen blocked arteries in some people experiencing an ischemic stroke, reducing the severity of the stroke and reversing some of its effects.
“Clot-busting medications given within three to four-and-a-half hours of symptom onset can help prevent lasting disability in up to one-third of patients,” says Shafie.
Stroke care revolutionized
Endovascular thrombectomy (EVT) is a breakthrough procedure UCI Health specialists use to treat stroke patients. A microcatheter (thin tube) is inserted through an artery in the patient’s groin, guiding it with X-ray imaging through blood vessels to the brain. There, a retrievable stent is used to remove large clots and restore blood flow.
EVT saves lives, reduces disability and is now considered the gold standard for treatment for patients with major ischemic strokes that involve large blood vessels in the brain. Initially EVT was approved only for patients within six hours of stroke symptom onset.
More recent clinical trials have shown that EVT can be performed safely and efficaciously within 24 hours after symptoms begin.
“The world of stroke care has been revolutionized in the past five to six years because of these advancements,” Shafie says. “EVT leads to very good outcomes for about half of stroke patients in that 24-hour window.”
Reducing your risk factors
During the pandemic, doctors have also been treating people who’ve delayed care for conditions that heighten risk of stroke. These include:
- High blood pressure: This is a major risk factor for both ischemic (blood clots blocking a blood vessel in the brain) and hemorrhagic (a blood vessel breaks and bleeds into the brain) stroke. Shafie encourages everyone — even those without a hypertension diagnosis — to check their blood pressure frequently with a home blood-pressure cuff and talk to their doctor about their readings.
- Physical inactivity: Getting 30 minutes of intense physical activity three or four times a week has a protective effect against stroke.
- High total cholesterol: Diet and lifestyle factors can help keep blood cholesterol at safe levels and lower the risk of fatty deposits building up in arteries. Medication can help when other measures fail.
- Diabetes: People who have had diabetes for more than three years have a 70% higher risk for stroke. Doctors say keeping hemoglobin A1c levels, a measure of blood sugar, to less than 7% can help control diabetes.
- Smoking: This triples or quadruples a person's risk for stroke. Even passive exposure to smoking increases risk.
- Atrial fibrillation: This type of irregular heart rhythm, which can increase with age and is more common among women, puts sufferers at high risk for stroke. Anticoagulants, when indicated, can reduce that risk by 50% to 60%.
- Obstructive sleep apnea: This risk factor for stroke can be evaluated with a sleep study. Treatment involves using a continuous positive airway pressure (CPAP) device to keep the air passage open during sleep.
- Obesity: This is also a risk factor for stroke. Diets that include fish, white meats, legumes, fruits and vegetables have been shown to help lose weight and protect against stroke.
- Alcohol: One glass of wine for women and two or fewer for men a day has a protective effect against ischemic stroke. Heavy alcohol use, however, can lead to bleeding in the brain as well as other detrimental impacts on overall brain health.
Shafie says studies show that "up to 90% of first strokes can be prevented with these risk-factor modifications.”
Expert care also makes a substantial difference in stroke prevention as well as better outcomes after a stroke. As part of an academic healthcare system, the stroke experts at UCI Health are actively engaged in translational research and clinical trials aimed at advancing knowledge in prevention, diagnosis and development of novel therapies to improve the lives of their patients.
The UCI Health Comprehensive Stroke & Cerebrovascular Center was among the first in Orange County and the nation to earn national certification by The Joint Commission, initially as a Primary Stroke Center and subsequently as a Comprehensive Stroke Center.
In recent years, the stroke team has been consistently recognized for the quality stroke and cerebrovascular care by the American Heart Association/American Stroke Association (AHA/ASA). The center has been awarded the association’s Target: Stroke Honor Role Elite Plus as well as Get with The Guidelines – Stroke Gold Plus.




