First UCI Health LVAD patient gets heart transplant
“I really want to continue being an advocate and mentor for LVAD and heart transplant patients,” says Elizabeth Vayssie, the third UCI Health patient whose left ventricular assist device (LVAD) kept her alive long enough to wait for a matching heart. Photo by Jared Novakovich for UCI Health
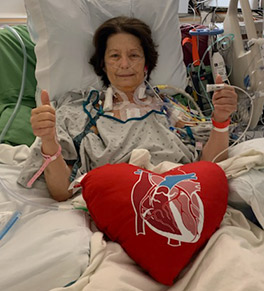
Elizabeth Vayssie heard the words every heart-failure patient hopes for: “We have a heart for you.”
The phone call last Oct. 30 came just 18 months after Vayssie became the first person in Orange County to receive a left ventricular assist device (LVAD), a life-saving surgery at UCI Health to pump blood through her body in place of her failing heart.
“My first thought was disbelief,” says the 59-year-old human resources professional. “I wasn’t expecting a call that soon because I’m a difficult match.”
That’s because she produces a high level of antibodies and receives regular infusions of immune globulin and blood plasma to regulate them and prevent rejection of a potential new heart.
The devoted baseball fan almost missed the call because she was so intent on watching game four of the 2021 World Series.
Diagnosis comes out of left field
An estimated 6.2 million Americans suffer from heart failure, causing about 309,000 deaths each year, according to the American Heart Association. Like many patients, Vayssie was shocked by her diagnosis in July 2019.
She’d blamed her symptoms — shortness of breath, an incessant cough, chronic fatigue — on other things. But once she showed up at UCI Medical Center's emergency department and described other symptoms such as tingling and numbness, a heavy feeling in her arms and neck, intermittent chest pain and abdominal bloating, heart tests were ordered immediately.
The ER team admitted Vayssie to the hospital, where her care was taken over by cardiologist Dr. Dawn Lombardo, founder and director of heart failure services at UCI Health and an expert in women’s heart disease. Lombardo’s diagnosis: advanced heart failure.
Covering the bases
Lombardo tried several proven drug therapies to improve Vayssie's heart condition, but low blood pressure due to her weakened heart meant she couldn’t tolerate even the smallest doses of medication. Implanting a pacemaker helped regulate increasingly irregular heartbeats for a time. But by March 2020, just as the pandemic shut down the world, her heart was too weak for traditional approaches.
“Elizabeth was in dire need of an LVAD to support her heart,” says Lombardo.
LVADs take over the pumping action of the heart muscle. One end of the pump is attached directly to the heart’s left chamber, called a ventricle, where blood flows through the aorta, the heart’s main artery, to the rest of the body. A tube called a driveline, connects the device through a hole in the abdomen to a smartphone-sized controller carried outside the body.
The devices have two primary uses: as a bridge while transplant patients wait for an available heart and as a long-term treatment for people who can’t have a transplant due to other medical conditions.
Fortunately for Vayssie, the UCI Health cardiothoracic surgery team had just established a vascular assist device (VAD) program for advanced heart failure patients. Spearheading the program is Dr. Fabio Sagebin, an expert in minimally invasive LVAD implant techniques that reduce surgical risks and complications, allowing patients to recuperate much faster.
On April 22, 2020, Sagebin successfully implanted the LVAD that saved Vayssie’s life. She was sitting up by nightfall, discharged in less than two weeks and returned to work part-time in six weeks. She was also put on the heart transplant list at Cedars-Sinai Medical Center in Los Angeles.
Stepping up to the plate
Life with the LVAD had its challenges, she says. Initially, it was hard to carry the 10-pound backpack housing her heart pump. Six months after surgery, she started monthly blood plasma infusions to help regulate her antibodies and make her eligible for a heart transplant. But the biggest obstacle was coping with premature ventricular contractions (PVCs), a type of heart arrhythmia that she had prior to the LVAD surgery. She became highly aware of their effect on her body after it was implanted.
“I was having a million extra heartbeats per week,” she says. “It made me so tired and the PVCs set off alarms, affecting my LVAD’s ability to fill completely.”
The cardiovascular team tried adjusting the LVAD but the arrhythmia continued. Next, they modified her medications, which only made her more tired. Ultimately, they programmed her pacemaker to completely take over the beating of her heart.
“I call them my team of angels,” Vayssie says. “The care I receive at UCI Health is phenomenal. They have been there for me 24/7 and I never feel alone.”
A home run
On Halloween 2021, the grandmother of three packed a bag and arrived at the hospital early in the morning. Her transplant surgery would happen that night if diagnostic tests confirmed a match.
As Vayssie waited in her room, she sent a text: “Dr. Lombardo, I’m at the hospital and they might have a heart for me!”
Lombardo called her back immediately. “I couldn’t just text you back. I had to talk to you!” the doctor told her.
At 9:30 p.m., Vayssie was wheeled into the operating room. Her family received updates from the surgical team throughout the night: at 3 a.m., the new heart is in; 5 a.m., in recovery; 7:30 a.m., in her room; 5:30 p.m., awake.
“When they woke me up, I’d been asleep 20 hours but it felt like a minute,” she recalls. A nurse removed her breathing tube and asked her to talk.
“I asked for my phone,” Vayssie says, laughing at the memory. “The nurse said she’d only had one other patient do that.”
The first thing she did was send a picture of herself post-surgery to Dr. Lombardo.
The next day, Katie Tran, a nurse and friend from the UCI Health advanced heart failure team, drove to Los Angeles to check on her.
“I was so happy to have my new heart but I started crying when I saw her,” says Vayssie. “I told her that my story wasn’t over, that I still want to be part of the VAD support group, to continue being an ambassador and give other patients hope.”
A few curveballs
Three months after surgery, Vayssie has much to celebrate. Her energy is back to normal and she’s sleeping better, and she is returning to work next week.
“The best thing is not carrying the LVAD around and being able to wear pants again,” she says.
She’s also thrilled to be able to take real showers and swim in a pool, things that were off limits given the risk of infection and the device, itself.
There are still challenges ahead. For the rest of her life, she’ll need to take medications to prevent her body from rejecting the new heart. She’s learning to manage their side effects and is hopeful the dosages can be reduced over time.
She's also learning to deal with her body’s delayed response to emotions and stress, the result of sympathetic nerve fibers being severed during heart transplant surgery. Emotions can hit her out of the blue.
“When I get angry and upset, it takes a while for my heart and nervous system to catch up and calm down,” Vayssie says. “My brain will be saying it’s over but my heart will still be pounding. That feels really weird.”
Nerve regeneration — called reinnervation — is possible but it can take months or years after surgery. It’s more likely to occur in cases involving young donors, young recipients and fast, uncomplicated transplant surgeries. Vayssie’s donor was an 18-year-old female and the transplant went well, so she’s hoping for the best.
She attends cardiac rehabilitation therapy three times a week and is looking forward to the time when she can workout in a gym to keep her body healthy and perhaps lessen the stress and anxiety she feels.
A whole new ball game
Vayssie is the first of 12 UCI Health patients who have received vascular assist devices and now she the third patient who has gone on to get a heart transplant thanks to the life-saving bridge treatment.
UCI Health does not currently perform heart transplants, but the advanced heart failure team works closely with partner hospitals in the region, providing pre-transplant workups, presenting patients at heart transplant selection committees and maintaining close communication with patients throughout the process. Usually within one year of their surgery, patients return to UCI Health for continued monitoring and support services.
Vayssie is extremely grateful to her heart donor’s family. Six months after the surgery, she’ll be allowed to write a letter of thanks and leave her contact information. She has also joined a Facebook group for heart transplant recipients.
“I really want to continue being an advocate and mentor for LVAD and heart transplant patients,” she says. “You can still have a good life after experiencing heart failure with the right team helping you. That’s what my UCI Health experience has taught me.”
Related Stories
- Heart patient gets lifesaving implant ›
- First LVAD recipient at UCI Health celebrates one-year anniversary ›
- Cardiothoracic surgeon describes how LVAD helps patients (video) ›
- Seven powerful ways to strengthen your heart ›