Flat polyps: Why finding them requires skill

Flat polyps are unwelcome news in the world of colonoscopy.
Raised polyps are well-recognized growths in the colon that gastroenterologists routinely remove before the abnormal tissue might turn into cancer.
They are easy to find and easy to remove.
But flat polyps are difficult for doctors to detect. They’re tougher to remove completely. Yet, they need to be found and removed because they can also turn into cancer and some may do so more quickly.
Fortunately, medicine is finding new ways to find and combat these troublesome polyps with better colonoscopy techniques and technology. Equally important, though, is heightened awareness among gastroenterologists who are learning how important it is to search carefully for flat polyps, as well as to refer patients to specialized colonoscopists to remove them.
“We’re now aware that these polyps exist,” said Dr. Jason Samarasena, a UCI Health interventional gastroenterologist with the H.H. Chao Comprehensive Digestive Disease Center (CDDC) and one of those specialized colonoscopists. “This is one of the most important concepts in colonoscopy right now.”
What are flat polyps?
Polyps are lesions found in the colon that are removed during colonoscopy. Many of them would never cause a serious health problem, but some are adenomas — precancerous growths that could turn cancerous over time.
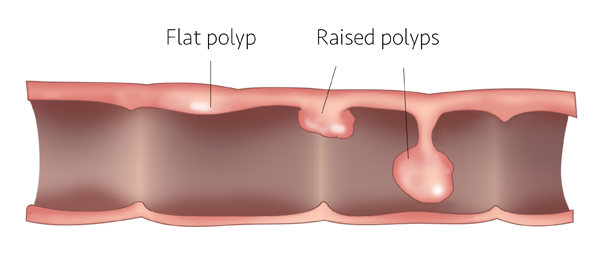
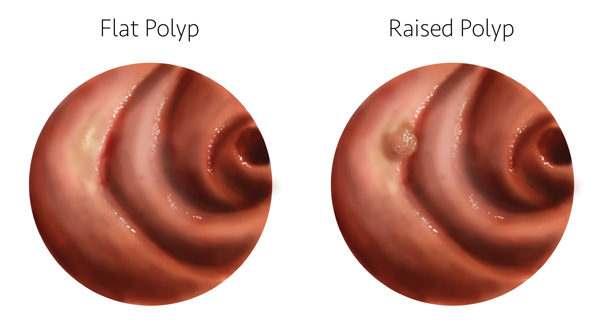
Most polyps look something like a mushroom growing from the colon wall, Samarasena said. They are easily seen during colonoscopy and, because the area where they touch the colon is small, they’re easily removed. Flat polyps, though, grow by spreading along the colon wall, usually in the right colon.
“The flat polyps are laterally spreading instead of growing tall,” Samarasena said. “They grow wide, and creep and creep and creep.”
Flat polyps are believed to make up about 9 percent of all polyps. Yet, because they are so difficult to find and remove completely, flat polyps are believed to be responsible for most of the colon cancers that occur in people who are up-to-date with their colonoscopies.
While 91 percent to 94 percent of colorectal cancers are diagnosed in people who are not up to date with their colonoscopies, 6 percent to 9 percent of colorectal cancers occur in people who are up-to-date.
Techniques and technology assist detection
CDDC doctors use several newer colonoscopy techniques to find these difficult-to-detect polyps. Dr. William Karnes, a UCI Health gastroenterologist who specializes in colorectal cancer screening, has been relying on “underwater” colonoscopy for the past couple of years.
Traditionally, colonoscopies have used air to create a kind of balloon within the colon, in order to better view the colon walls. But that has its downsides.
“When you use air, you stretch the colon wall,” Karnes said. “So the flat polyp flattens even further, making it even harder to see.”
Underwater colonoscopy fills the colon with water, which offers several advantages:
- It cleanses the colon walls during the examination.
- The mucosa — the top layer of the colon’s lining — floats up a little in the water, making the flat polyp easier to find, Karnes said.
- Side benefit: No gas pain for patients, unlike for patients whose colons were pumped full of air.
High-resolution scopes give a clear view of small clusters of cells, allowing for a detailed colonoscopy.
High-resolution scopes improve polyp detection
Karnes also uses high-resolution scopes that give him a clear view of minute clusters of cells. All of this aids him in his meticulously detailed examination of the colon walls during colonoscopies.
“In old days we couldn’t see the flat polyps because the resolution wasn’t clear enough,” he said.
“I can’t tell you how many times I’ve gone up and down the right colon, I think I’ve seen every last bit. And I’m coming out, and suddenly, there it is, a polyp. It raises the hair on the back of my neck, to think I could have missed it.”
New medical devices also help. CDDC doctors use a device with soft fingers at the tip of the scope that gently spread and probe the walls of the colon as the scope is being withdrawn, turning over folds in the lining that might have been hiding polyps. Ask a gastroenterologist about colon cancer detection and prevention during our Facebook Live ›
Removing flat polyps
Karnes and other doctors often remove flat polyps when they’re small. But for larger lesions, they often call on Samarasena, who performs many such polypectomies each year.
The larger flat polyps need to be sectioned and removed piece by piece, he said, a long, painstaking procedure. The risks are higher than with removing regular polyps, carrying a greater chance of perforating the colon. It’s a task many gastroenterologists don’t feel comfortable undertaking.
And it can be hard to tell where the polyp ends and healthy tissue begins, which makes it difficult to ensure that the entire polyp has been removed, Samarasena said.
He sometimes injects blue-dyed saline solution into the layer of the colon beneath the area of the polyp. The blue color shows through the healthy tissue, but is blocked by the polyp, giving him a clearer view of the margins.
Even with all this care, in up to 30 percent of cases, not all of a flat polyp will be removed, so patients always return for a recheck in three to six months.
Know your doctor’s adenoma detection rate
How can patients know whether they’re getting the best colonoscopies possible? Karnes suggests asking the doctors for their adenoma detection rate.
In other words, in how many patients are adenomas found? Colonoscopists vary widely in their ability to find adenomas, ranging from 7 percent to 50 percent, Karnes said.
Medicare expects 25 percent detection among women and 30 percent among men.
It’s believed that 50 percent of patients have these lesions, so getting as close to that number as possible is important. Among UCI Health doctors, the numbers are above 43 percent and 58 percent respectively, Karnes said.
Similarly, he said, UCI Health’s detection rate for adenomas from flat polyps is 9.3 percent, compared with a national mean of 2 percent.
“The adenoma detection rate is one of the key quality measures,” Karnes said. “A lot of colonoscopists don’t know their rates, but with new rules by Medicare, they’re going to have to know by the end of this year.”




